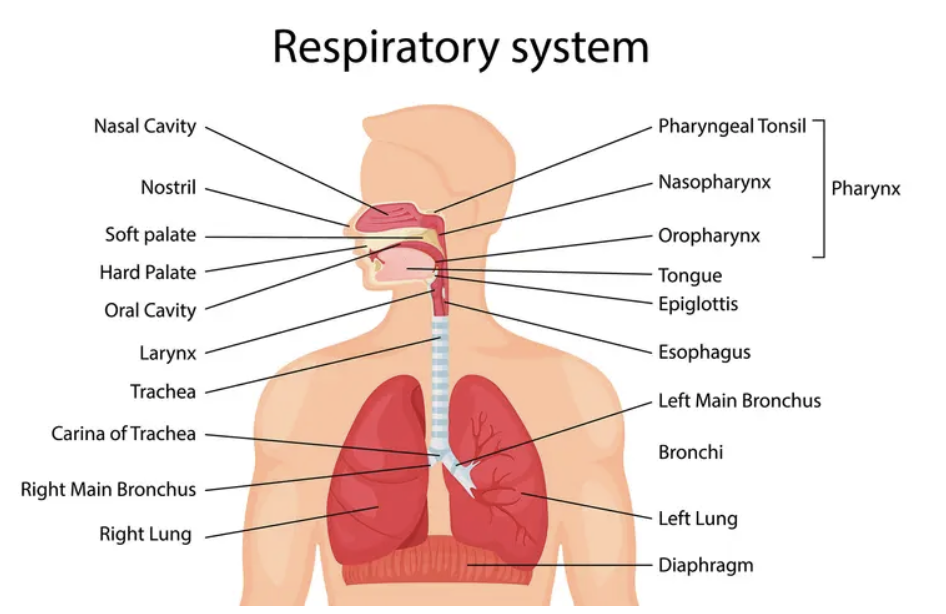
Common Respiratory Emergencies in Sports
Introduction:
Breathing is one of the fundamental requirements for athletic performance. Maintaining a consistent oxygen supply throughout the bloodstream is essential for energy production, endurance, and overall health. Because breathing is so important, respiratory emergencies in sports can escalate rapidly and become life-threatening if not addressed immediately. For athletes, family members, and coaches, understanding common respiratory emergencies is critical for both performance and survival.
Asthma:
Asthma, or exercise-induced bronchoconstriction (EIB), is one of the most common conditions, causing the bronchioles to swell and excess mucus production, which prevents proper ventilation from occurring.
Signs and Symptoms
Shortness of breath (dyspnea)
Wheezing (inspiratory and expiratory)
Decreased or absent lung sounds
Persistent coughing
Early fatigue
Tightness in the chest
Treatment
Administer bronchodilators such as albuterol inhalers
Maintaining calm, controlled breathing
Call emergency medical services if symptoms worsen
Prevention
Using prescribed inhalers before physical activity
Avoiding triggers (allergens, cold air, pollution)
Regulatory checkups for respiratory evaluations
Anaphylaxis:
Anaphylaxis is a severe allergic reaction that can cause rapid swelling of the airway. This condition is a medical emergency and requires medical services to be called immediately. In sports, anaphylaxis is often triggered by allergens such as insect stings, food, and medications.
Signs and Symptoms
Hives/urticaria (raised, red, and itchy bumps along the skin)
Swelling of the throat, lips, or tongue
Difficulty swallowing and breathing
Stridor/wheezing
Dizziness and loss of consciousness
Treatment
Administer epinephrine (EpiPen)
Call emergency medical services
Place the athlete on their back (supine) with legs elevated
Prevention
Identifying known allergies
Ensure epinephrine availability (usually through an EpiPen)
Airway Obstruction:
Airways can become obstructed from a variety of factors, including blood, vomit, foreign bodies, or trauma to the neck or face. This is more common in contact sports where athletes risk trauma to their respiratory system.
Signs and Symptoms
Gasping or clutching the throat
Inability to cough or speak
Cyanosis (bluish skin or lips)
Loss of consciousness
Treatment
Heimlich maneuver (abdominal thrusts) if the athlete is conscious
Perform CPR if they become unresponsive
Calling emergency medical services to suction the airway and provide oxygen
Prevention
Wearing proper gear for contact sports (mouthguards, helmets, etc.)
Avoid chewing gum or eating during the activity
Pneumothorax:
Blunt chest trauma can damage lung tissue, causing a leakage of air into the chest cavity. This collapses the lungs and prevents proper breathing, creating a life-threatening situation. These injuries are much more common in high-impact sports.
Signs and Symptoms
Sharp chest pain on one side
Shortness of breath (dyspnea)
Unequal chest expansion
Low oxygen saturation
Rapid breathing
Treatment
Immediately call emergency medical services
Place the athlete flat on their back (supine)
Provide supplemental oxygen if available
Chest tube placement in severe cases
Prevention
Wearing proper padding and protective gear
Enforcing rules to ensure athlete safety
Hyperventilation Syndrome:
Characterized by excessively rapid breathing, hyperventilation disrupts the balance between oxygen and carbon dioxide in the body. It is often caused by stress, anxiety, and overexertion.
Signs and Symptoms
Rapid breathing
Dizziness
Panic attacks
Tingling sensation in hands and feet
Chest tightness
Treatment
Remove athletes from stressful stimuli
Reassurance and maintaining a calm attitude
Guide slow, controlled breathing
Providing supplemental oxygen (if possible and after breathing is stabilized)
Constantly monitoring vital signs
Prevention
Breathing control training
Stress management technique
Mental health support
Conclusion:
In sports, respiratory emergencies require rapid recognition to provide immediate life-saving treatment. Responders must remain calm and collected, calling for emergency medical services immediately and providing supportive care before they arrive. An athlete’s ability to breathe is crucial not only to their athletic performance but also for survival, making respiratory safety a top priority no matter the environment.
Sources:
“Airway Obstruction.” Cleveland Clinic, https://my.clevelandclinic.org/health/diseases/airway-obstruction.
“Anaphylaxis — Symptoms & Causes.” Mayo Clinic, https://www.mayoclinic.org/diseases-conditions/anaphylaxis/symptoms-causes/syc-20351468.
“Asthma — Symptoms & Causes.” Mayo Clinic, https://www.mayoclinic.org/diseases-conditions/asthma/symptoms-causes/syc-20369653.
“Collapsed Lung (Pneumothorax).” Cleveland Clinic, https://my.clevelandclinic.org/health/diseases/15304-collapsed-lung-pneumothorax.
“Hyperventilation.” Cleveland Clinic, https://my.clevelandclinic.org/health/diseases/hyperventilation.
“Effects of Chest Trauma on the Lungs.” PMC (PubMed Central), https://pmc.ncbi.nlm.nih.gov/articles/PMC4952126.